How Technology Can Bridge the Rural Health Divide
Part 3 of the Rural Health Resilience Series (Read Part 1 and Part 2 Here)
Rural America faces persistent health challenges—shortages of clinicians, long distances to care, and aging facilities. But new policies, infrastructure investments, and technological innovations are laying the groundwork for a healthier future.
The recently passed One Big Beautiful Bill Act includes the Rural Health Transformation Program, a $50 billion federal initiative providing $10 billion annually from 2026–2030 to states with qualifying transformation plans. This funding is designed to modernize rural care by supporting broadband expansion, digital infrastructure, chronic disease management, and training for technologies such as artificial intelligence (AI) and remote patient monitoring.
While this investment is meant to offset the Act’s Medicaid spending cuts and other reimbursement reductions that will disproportionately touch rural providers, it also demonstrates an increased awareness that brick and motor care centers must be magnified in reach and scope via transformative technology adoption. Digital solutions must play a central role in the future of rural health.
Building the Digital Foundation
Before AI and other innovations can transform rural health, the basic infrastructure must be in place. This includes:
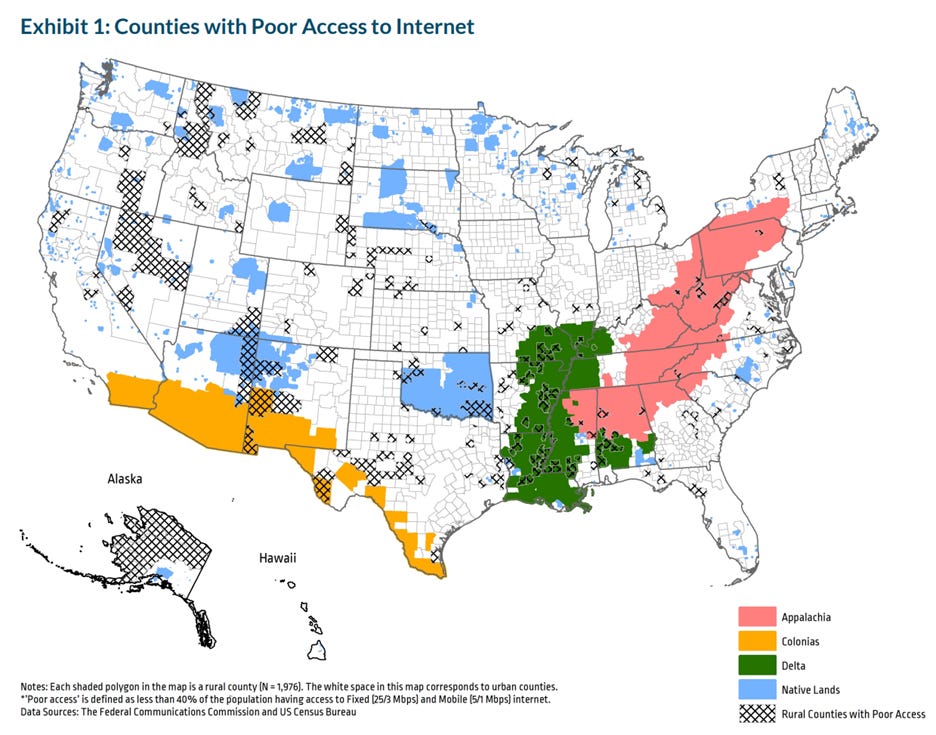
High-speed broadband reaching homes, clinics, and mobile care units.
Secure, cloud-based systems for clinical data sharing.
AI governance frameworks to ensure tools are safe, explainable, and equitable.
Training programs to help clinicians, administrators, and patients use new technologies confidently.
Some organizations are already acting. For example, Thrive Health Tech* equips patients with mobile devices connected to secure networks, bridging broadband gaps. Major tech companies are beginning to partner with rural hospitals to modernize cybersecurity and electronic health record systems.
AI in Action: Practical Solutions for Rural Communities
Once the foundation is set, AI-enabled tools can deliver tangible benefits:
1. Supporting Patients and Extending In-Home Care
AI-powered platforms provide personalized health education, explain care plans in plain language, and work across literacy levels and languages. Paired with remote monitoring, they create a continuous link between patients and providers.
Companies like Sprinter Health send trained clinicians to patients’ homes in rural areas, using AI-powered logistics to optimize travel routes. These visits, often paired with virtual nurse practitioner consults, help patients access timely care without long travel.
2. Giving Clinicians Time Back
Rural clinicians face heavy administrative burdens. AI tools streamline documentation, coding, and prior authorizations. For example, Ambience Healthcare’s* AI-enabled “ambient scribes” reduce documentation time by 40%, freeing up time for patient care and improving billing accuracy.
3. Making Operations Smarter
AI can automate scheduling, eligibility checks, and insurance workflows. CodaMetrix* has shown a 70% reduction in manual coding work and fewer costly denials through automation, helping rural facilities remain financially viable.
4. Extending Expertise Through Virtual Consultation
AI-powered diagnostic support tools help rural clinicians manage complex cases without on-site specialists. In radiology, vision models can triage imaging studies, flagging urgent cases. Partnerships like OpenAI’s work with Kenya’s Penda Health, show measurable improvements in diagnostic accuracy— a 16% reduction in diagnostic errors over 40,000 patient visits—benefits that can translate to U.S. rural settings.
Ensuring Safe and Trusted AI
Innovation must be paired with safeguards. Rural facilities often have limited IT resources, making clear AI governance essential. Platforms like Qualified Health* give providers real-time performance monitoring, audit trails, and safety frameworks to ensure AI systems are reliable and transparent. The tools must be explainable, tested for bias, and work consistently across diverse populations and care settings.
These guardrails—combined with community trust and involvement—are key to sustainable adoption.
A Future of Connection, Not Just Proximity
The Rural Health Transformation Program is limited in size and will not solve for the array of challenges our rural health care systems face – including new difficulties arising from the One Big Beautiful Bill’s Medicaid cuts. But it signals a shift: rural health care matters, and technology can help make it more accessible, equitable, and sustainable.
The future of rural health will rely less on large inpatient facilities and more on connected networks—care delivered in homes, local clinics, and mobile units, supported by secure digital infrastructure and AI-driven efficiency.
Rural America’s tradition of resilience and resourcefulness positions it to lead this transformation. Just as mobile technology leapfrogged landlines in parts of the world, rural health can bypass outdated models and move directly into a connected, patient-centered era.
With the right policies, partnerships, and technology, rural communities can shape a health care system that is smarter, earlier, and more personal—delivering care without distance.
Frist Cressey Ventures, of which the author is a partner, has a minority investment in the companies marked with an asterisk above. They are for illustrative purposes only.
Read more on this by the author at Forbes: https://www.forbes.com/sites/billfrist/2025/08/14/care-without-distance-rural-healths-leap-into-the-digital-age/



Sadly, these initiatives should be in addition to onsite health care, not a replacement. They cannot address the person to person relationship between an onsite caregiver and patient, so important to better compliance and outcomes. They won’t help the emergent, be that the massive stroke patient, the OB patient with complications, the acute MI and on and on. There is no sense of community necessary for a quality life. The art of medicine, the real basis for holistic care, is completely lost. I am a big believer in all of these tools as adjunct additions. But it will never be medical CARE. It is nothing short of discriminatory. It surely doesn’t represent the possibilities for a nation that can rise to the top, become leaders and set a standard. It’s a reaction built on profits for one sector and loss of humanity for the rest.